What is a Hypertensive Crisis?
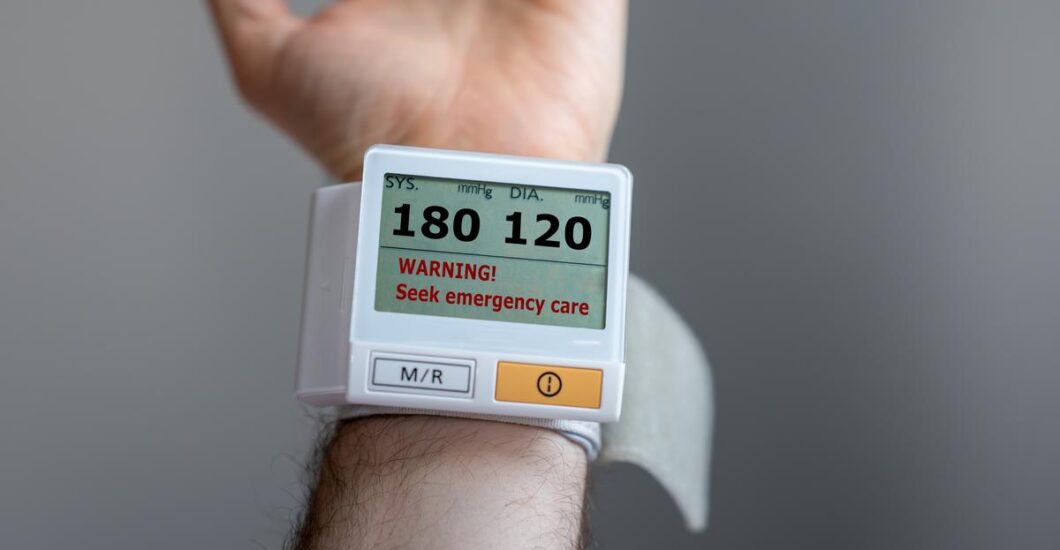
A hypertensive crisis, also known as a hypertensive emergency, is a severe condition characterized by a sudden and significant increase in blood pressure. During a hypertensive urgency, blood pressure readings rise to dangerously high levels, typically exceeding 180/120 mmHg.
This condition requires immediate medical attention as it can pose serious risks to various organs, including the heart, brain, kidneys, and blood vessels. Uncontrolled high blood pressure can potentially lead to life-threatening complications such as heart attacks, strokes, kidney damage, and even heart failure.
Types of Hypertensive Crisis
There are two main types of hypertensive crisis: hypertensive emergency and hypertensive urgency.
- Hypertensive Emergency:A hypertensive emergency is a severe and potentially life-threatening condition characterized by extremely high blood pressure levels along with evidence of organ damage. This type of crisis requires immediate medical attention and hospitalization. Organ damage can affect various systems, including the heart, brain, kidneys, and blood vessels. Symptoms may include hypertension headaches, chest pain(angina), shortness of breath, blurred vision, dizziness, confusion, seizures, and unresponsiveness. Hypertensive emergencies can lead to serious complications such as heart attacks, strokes, kidney failure, or aortic dissection. Emergency medical treatment is necessary to rapidly lower blood pressure and prevent further damage.
- Hypertensive Urgency:Hypertensive urgency is a condition characterized by an elevated blood pressure without evidence of acute organ damage. Although blood pressure levels are dangerously high, there is no immediate threat to organ function. However, prompt medical evaluation and treatment are still necessary to prevent the progression to a hypertensive emergency. Hypertensive urgency can cause severe headaches, nosebleeds, shortness of breath, anxiety, and dizziness. Treatment typically involves close monitoring, medication adjustment, and lifestyle modifications to bring blood pressure under control and reduce the risk of complications.
Symptoms of Hypertensive Crisis
While the symptoms can vary depending on the individual and the extent of organ involvement, there are several common signs and symptoms associated with hypertensive crises:
- Severe headache: One of the most common symptoms experienced during a hypertensive crisis is a severe headache. The headache may be described as intense, throbbing, or pulsating.
- Shortness of breath: Difficulty breathing or shortness of breath can be a sign of a hypertensive crisis. It may occur at rest or with minimal exertion.
- Chest pain: Chest pain or discomfort can occur during a hypertensive crisis. It may be experienced as pressure, tightness, or a squeezing sensation in the chest. The pain may radiate to the shoulders, arms, neck, jaw, or back.
- Dizziness or lightheadedness: Feeling dizzy or lightheaded is a common symptom associated with hypertensive crises. It may be accompanied by a sensation of spinning or imbalance.
- Blurred vision: Vision problems, such as blurred vision or visual disturbances, can occur during a hypertensive crisis. This may manifest as seeing spots, flashes of light, or experiencing temporary vision loss.
- Nausea or vomiting: Some individuals experiencing a hypertensive crisis may also experience nausea or vomiting. These symptoms can be attributed to the strain that high blood pressure places on the body’s organs.
- Seizures or confusion: In severe cases of hypertensive crises, seizures or a state of confusion may occur. These symptoms indicate a critical situation and require immediate medical attention.
Causes of Hypertensive Crisis
Understanding the causes is important in order to effectively manage and prevent hypertensive crises. Here are some common causes:
- Medication non-compliance: Failing to take prescribed antihypertensive medications as directed or missing doses can lead to uncontrolled blood pressure and increase the risk of a hypertensive crisis.
- High blood pressure fluctuations: Rapid and significant fluctuations in blood pressure levels can contribute to a hypertensive crisis. This can occur in individuals with poorly controlled hypertension or those with certain medical conditions.
- Medication side effects: Certain medications or drug interactions can cause a sudden increase in blood pressure, leading to a hypertensive crisis. This may include medications such as nonsteroidal anti-inflammatory drugs (NSAIDs), oral contraceptives, decongestants, or certain herbal supplements.
- Illicit drug use: The use of illicit drugs, such as cocaine, amphetamines, or certain stimulants, can cause a sudden and severe increase in blood pressure, triggering a hypertensive crisis.
- Kidney problems: Kidney disease or kidney dysfunction can disrupt the body’s fluid and electrolyte balance, leading to increased blood pressure. Conditions such as renal artery stenosis or acute kidney injury can contribute to hypertensive crises.
- Endocrine disorders: Certain endocrine disorders, such as adrenal gland tumors (pheochromocytoma) or hyperthyroidism, can cause fluctuations in blood pressure and increase the risk of hypertensive crises.
- Acute stress or emotional distress: Intense emotional stress or acute psychological distress can temporarily elevate blood pressure levels and potentially trigger a hypertensive crisis, especially in individuals with existing hypertension.
- Certain medical conditions: Certain medical conditions, such as aortic dissection, eclampsia in pregnancy, or acute glomerulonephritis, can lead to a sudden increase in blood pressure and result in a hypertensive crisis.
Hypertensive Crisis Treatment & Prevention
The treatment and prevention of hypertensive crises focus on swiftly lowering blood pressure levels and addressing the underlying causes. If you or someone experiences a hypertensive crisis, it is important to seek immediate medical attention.
Here are common approaches to treatment and prevention:
- Hospitalization: In most cases, hospitalization is required for close monitoring and administration of appropriate medications to bring down blood pressure safely and effectively. During your hospital stay, your doctor may also perform additional tests, such as an echocardiogram, to assess the structure and function of your heart and gather more information about your cardiovascular health.
- Medications: Medications known as antihypertensives are used to lower blood pressure during a hypertensive crisis. The specific medication and route of administration will depend on the severity of the crisis and individual patient factors. Intravenous medications like nitroprusside or labetalol are commonly used.
- Fluid balance: Maintaining proper fluid balance is crucial during a hypertensive crisis. Fluids may be given intravenously to ensure adequate hydration while avoiding excessive fluid intake that can further increase blood pressure.
- Addressing underlying causes: If a specific cause or trigger for the hypertensive crisis is identified, such as medication non-compliance or illicit drug use, appropriate measures will be taken to address and manage the underlying condition.
- Lifestyle modifications: After a hypertensive crisis, healthcare providers will emphasize the importance of lifestyle modifications to prevent future crises. This includes following a healthy diet low in sodium, engaging in regular physical activity, managing stress levels, maintaining a healthy weight, and avoiding tobacco and excessive alcohol consumption.
- Regular blood pressure monitoring: Ongoing monitoring of blood pressure is crucial to ensure it remains within a healthy range. Regular check-ups with a healthcare provider, including the use of diagnostic tools like an echocardiogram, are important for adjusting medications, assessing overall cardiovascular health, and detecting any underlying cardiac abnormalities.
- Medication adherence: It is vital to strictly adhere to prescribed antihypertensive medications to control blood pressure and prevent future hypertensive crises. Taking medications as directed and attending follow-up appointments with the healthcare provider is essential.
- Stress management: Managing stress through techniques like relaxation exercises, mindfulness, and engaging in activities that promote emotional well-being can help prevent spikes in blood pressure.
- Education and support: Understanding the signs and symptoms of a hypertensive crisis and having a support system in place can help individuals and their loved ones respond promptly and appropriately in case of an emergency.
In a Nutshell
Dealing with a hypertensive crisis requires immediate medical attention to ensure prompt and appropriate treatment. The condition necessitates hospitalization for close monitoring, administration of medications, and comprehensive care.
If you have concerns about your blood pressure or need assistance in managing hypertension, it is crucial to connect with a qualified healthcare professional. If you want to find a skilled physician near you you can visit our Find a Physician page and connect with a healthcare provider who is experienced in managing hypertension and other related conditions. They can provide personalized guidance, monitor your condition closely, and help you develop a comprehensive treatment plan.
Don’t hesitate to reach out and take control of your health.
Disclaimer
The information contained in this article is to educate, spread awareness in relation to hypertension and other diseases to the public at large. The contents of this article are created and developed by BPinControl.in through its authors, which has necessary, authorisations, license, approvals, permits etc to allow usage of this articles on The Website. The views and opinions expressed in this article are views, opinions of the respective authors and are independently endorsed by doctors. Although great care has been taken in compiling and checking the information in this article, The Website shall not be responsible, or in any way liable for any errors, omissions or inaccuracies in this article whether arising from negligence or otherwise, or for any consequences arising therefrom. The content of this article is not a substitute for any medical advice. The Website shall not be held responsible or liable for any consequence arising out of reliance on the information provided in the article.